,
by Carmen Phillips
Scientists have devised a possible new technique for treating most cancers by taking the flexibility of tumors to quickly evolve and turning it in opposition to them.
The actual evolutionary change they’re focusing on is tumors’ uncanny capability for making tiny modifications of their organic make-up that may trigger a most cancers drug that had been working to cease doing so—a phenomenon typically referred to as therapy resistance.
However the researchers, from Penn State, have provide you with a method to benefit from this troublesome adaptation. And, surprisingly, it includes deliberately engineering most cancers cells inside a tumor to be proof against a selected therapy from the get-go.
Their thought is that as a affected person undergoes therapy, the engineered most cancers cells don’t simply survive, they thrive, shortly taking up the tumor. And that’s when the tables flip, as a result of those self same most cancers cells are additionally engineered to have a second ability: producing a drug that kills each them and different close by, nonengineered most cancers cells.
By giving or stopping using particular medication, the engineered cells’ new talents will be turned on and off like gentle switches, defined the examine’s lead investigator, Justin Pritchard, Ph.D., of Penn State’s Huck Institutes of the Life Sciences.
In experiments in mouse fashions of lung most cancers, the method labored exactly as hoped, with tumors being utterly eradicated and showing to not return. The examine, funded partly by NCI and several other different NIH institutes, was revealed July 4 in Nature Biotechnology.
Khalid Shah, Ph.D., director of the Heart for Stem and Translational Immunotherapy at Brigham and Ladies’s Hospital, who has led analysis on engineering most cancers cells to make use of them as most cancers remedy, referred to as the outcomes “promising.” The findings, Dr. Shah mentioned, present robust proof it’s doable to “ahead engineer the evolution of tumor cells.”
“We all know that it’s a distinct approach” to consider treating most cancers, Dr. Pritchard mentioned. However with these promising preliminary outcomes, he continued, their group looks like “there are lots of alternatives right here.”
The evolution of therapy resistance
Remedy resistance is among the many greatest challenges in most cancers, with some research estimating that it contributes to 80% to 90% of cancer-related deaths.
Most cancers cells that develop into proof against a therapy, or which are naturally resistant, are very similar to a handful of weeds in a garden that, not like others within the yard, aren’t killed by weed spray from the native ironmongery store. In a matter of days or even weeks, these few cussed weeds can seed lots of buddies all through the garden.
Equally, in tumors, most cancers cells which are delicate to a therapy are killed off, whereas people who have the organic wherewithal to resist these assaults stay. These resistant cells then begin multiplying and the tumor resumes rising.
Exactly how particular person tumors develop into resistant can fluctuate from individual to individual, however typically there are frequent mechanisms—most frequently new genetic modifications—that most cancers cells purchase. That is significantly true for resistance to focused therapies, which characterize the overwhelming majority of latest most cancers medication accepted by the Meals and Drug Administration over the previous 25 years.
For instance, focused therapies work by latching on to a part of a mutated protein on or inside most cancers cells, which in flip creates a cascade of occasions that causes the cells to die.
However as tumors are barraged by these therapies, over time some cells within the tumor develop extra genetic mutations that trigger the form of the proteins at these exact binding spots to alter. When that occurs, the medication can not seize on to their protein targets on these cells, and shortly sufficient the remedies cease working altogether.
The answer to this downside has been for researchers to develop new types of focused therapies (typically referred to as second- and third-generation medication) that may work even when resistance-inducing genetic modifications are current in these cells.
Many of those next-generation therapies “are nice medication,” Dr. Pritchard mentioned. However, he added, tumors virtually all the time discover a method to outwit them too.
Redirecting tumor evolution
The Penn State group determined to revisit this “reactive” technique to combatting resistance. As an alternative of ready to see how tumors evolve to flee the assaults of a given therapy, they thought, why not “redirect” evolution and use it of their favor?
To tug off this redirection, they might use genetic engineering expertise to insert two completely different genes into most cancers cells within the lab that may give them particular talents.
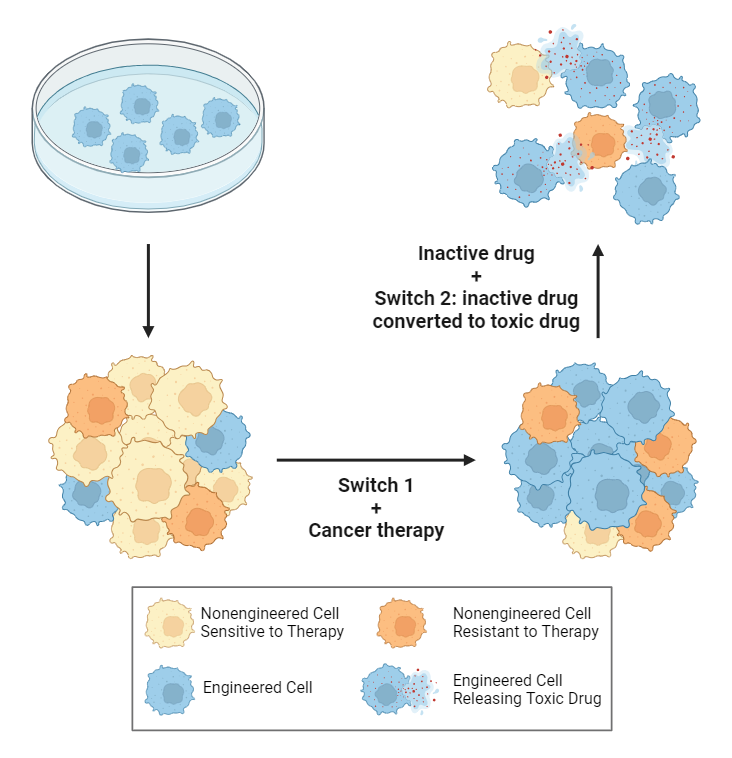
The primary gene, or swap 1, supplies the directions for making the cells proof against a selected therapy.
The second gene, or swap 2, transforms the cells into “native drug factories,” offering the directions for remodeling an inactive drug right into a poisonous drug. After killing the most cancers cells, that poisonous drug can also be dispersed into their close by environment, killing different most cancers cells within the quick space.
For the technique to work, this collateral injury—or bystander impact—to close by most cancers cells is crucial, wrote Andriy Marusyk, Ph.D., who research most cancers evolution at Moffitt Most cancers Heart in Tampa, FL, in an editorial that accompanied the examine.
The bystander impact “maximizes the chances of” eliminating nonengineered most cancers cells, Dr. Marusyk wrote, but in addition “engineered cells through which [the gene for switch 2] was misplaced or inactivated by mutations.”
Eliminating tumors in mice
To check the feasibility of their thought, Dr. Pritchard and his group started through the use of pc fashions that allowed them to higher perceive how tumors evolve in response to completely different remedies. These fashions, and a few laboratory experiments, additionally helped them simulate the affect of their technique in numerous most cancers sorts utilizing completely different therapies and gene designs for the switches.
An enormous a part of this work, Dr. Pritchard mentioned, was “enthusiastic about all of the other ways this [strategy] may go improper.”
From there, they once more used the pc mannequin to assist design a swap technique for a typical therapy state of affairs: lung most cancers with mutations within the EGFR gene being handled with the third-generation EGFR-targeted remedy osimertinib (Tagrisso). Though research present that therapy with osimertinib shrinks tumors for prolonged intervals in about 70% of individuals handled with it, resistance invariably units in and the tumors resume rising.
They then examined the technique in mice. To get the engineered cells into tumors, each engineered and nonengineered EGFR-mutated most cancers cells (together with these naturally proof against osimertinib) had been implanted into mice, which briefly order shaped into tumors.
Change 1 was turned on by giving the mice a drug referred to as a dimerizer, whereas swap 2 was turned on by the inactive drug that may be changed into a toxin.
Preliminary experiments confirmed that the technique shrank tumors and appeared to have the specified bystander impact. For the ultimate experiments, the groups developed mice with tumors that higher simulate these in people, in that that they had extra cells that had been naturally proof against osimertinib.
Ten mice weren’t implanted with any engineered most cancers cells and 12 had tumors that did kind partly from implanted engineered cells.
Within the group of 10 mice, therapy with osimertinib initially shrank tumors in all of them. However the tumors quickly started rising once more and all of the mice shortly died. In contrast, 11 of 12 mice with engineered cells of their tumors had been alive a number of months after beginning therapy with osimertinib with no apparent proof that the tumors had began rising once more.
The problem of transferring from the lab to sufferers
There’s much more analysis to be executed, Dr. Shah mentioned. However this preliminary work reveals that it’s doable to pressure “drug resistance in a path that’s extra favorable for therapy versus permitting tumors to develop resistant [cancer cell] populations randomly.”
Transferring this concept from success in mice to testing in people will probably be tough, Dr. Pritchard acknowledged. Though there are a number of obstacles, he believes the largest “is supply”—that’s, getting the engineered most cancers cells into tumors.
As an alternative of engineering cells within the lab after which giving them again to sufferers, one potential possibility, Dr. Marusyk famous, includes a lesson from COVID vaccines: utilizing mRNA expertise to ship the directions for the switches on to tumors.
With continued advances in numerous methods of transferring genetic data into cells, he wrote, getting the switches into most cancers cells within the physique “will not be an insurmountable problem.”
Dr. Shah pointed to different potential hurdles. For instance, the proportion of cells in a tumor which are inherently proof against a given therapy is a vital consideration, he continued. Ranges of those cells “fluctuate throughout completely different tumor sorts and sufferers,” he defined, and can seemingly have an effect on the engineered cells’ means to take over a tumor.
So, getting the right combination of engineered cells to resistant cells in a given tumor will probably be “essential for the technique’s success,” Dr. Shah mentioned.
In keeping with Dr. Pritchard, the Penn State researchers are transferring ahead with testing methods for delivering the genes for the switches to tumors and fine-tuning the method in additional superior animal fashions. They’re additionally contemplating which varieties of cancers can be greatest to give attention to initially in future human research.
“We’re enthusiastic about that rather a lot,” Dr. Pritchard mentioned. Given the distinctive nature of their technique, he continued, deciding on the precise state of affairs for preliminary human research “will probably be crucial.”