Introduction
In keeping with the worldwide statistics launched by the Worldwide Company for Analysis on Most cancers in 2022, the brand new instances of colorectal most cancers (CRC) accounted for 9.6% of the brand new instances of malignant tumors on this planet yearly, rating second solely to breast and lung most cancers in ladies. Furthermore, CRC-related deaths accounted for 9.3% of cancer-related deaths, making it the second main reason behind most cancers mortality after lung most cancers (1–4).
These days, power kidney illness (CKD) has turn out to be a world public well being drawback, and Asia has one of many highest prevalence of CKD (5–7). In keeping with statistics, in 2019, there have been 9.8 million new CKD instances and 763,024 CKD-related deaths in Asia (8, 9).
A number of research have proven that CKD was considerably related to an elevated incidence of CRC (10–12). Nevertheless, the exact impact of CKD on postoperative problems and prognosis in CRC stays a topic of debate. Whereas Currie A et al. instructed that CKD sufferers may be extra more likely to develop cardiovascular problems after CRC resection and had an elevated danger of disease-free survival (DFS) (13); Huang CS et al. discovered that the CKD group had a considerably decrease 3-year DFS fee in comparison with the Non-CKD group (14); Furthermore, Nozawa H et al. concluded that CKD had little impact on total survival (OS) in TNM stage III CRC sufferers (15).
As earlier research reported, it was unclear the impact of CKD on postoperative problems and prognosis in CRC, Due to this fact, the aim of the present examine was to investigate the impact of CKD on the short-term outcomes and prognosis of CRC sufferers present process major surgical procedure for CRC.
Strategies
Sufferers
CRC sufferers who underwent radical surgical procedure have been included from Jan 2011 to Jan 2020 in a single scientific educating hospital. This examine was carried out following the World Medical Affiliation Declaration of Helsinki. And this examine obtained Moral approval from the institutional assessment board (The First Affiliated Hospital of Chongqing Medical College, 2024–010-01). All sufferers taking part within the examine obtained written knowledgeable consent.
Inclusion and exclusion standards
Sufferers who underwent major CRC surgical procedure have been included on this examine (n=5473). The exclusion standards have been as follows: 1, sufferers with incomplete scientific info (n=323); 2, non-R0 surgical procedure (n=25); 3, stage IV CRC (n=875); and 4, incomplete renal operate examination (n=194). Lastly, a complete of 4056 sufferers have been included on this examine. The flowchart and inclusion and exclusion standards have been proven in Determine 1.
Surgical procedure administration and follow-up
All included sufferers underwent whole mesorectal resection or whole mesocolic resection primarily based on the oncological rules, with postoperative pathology confirming R0 resection. Routine follow-up was carried out after surgical procedure: each three months for 3 years, and each six months thereafter.
Definitions
We used the Continual Kidney Illness Epidemiology Collaboration (CKD-EPI) creatinine equation to calculate eGFR to evaluate renal operate in all of the included sufferers. The CKD-EPI equation was gender-specific, and the precise method was as follows: eGFR = 141 × min (Scr/κ, 1)α × max (Scr/κ, 1)- 1.209× 0.993 Age× 1.018 [if female], the place Scr was serum creatinine, κ was 0.7 for females and 0.9 for males, α was −0.329 for females and −0.411 for males, min indicated the minimal of Scr/κ or 1, and max indicated the utmost of Scr/κ or 1 (16, 17). CKD was outlined as persistent proteinuria or eGFR<60ml/min/1.73m2 (18), subsequently, we outlined sufferers with eGFR< 60ml/min/1.73m2 because the CKD group and people with eGFR≥ 60ml/min/1.73m2 because the Non-CKD group. The pathological staging of tumors was principally primarily based on the AJCC eighth version analysis (19). Problems have been outlined in response to the Clavien- Dindo classification (20) and main problems have been outlined as Clavien- Dindo classification ≥ III problems. III Problems Contains problems requiring surgical, endoscopic, or radiologic intervention; OS was outlined because the time from the date of surgical procedure to the person sufferers’ loss of life of any trigger or the final follow-up time; DFS was outlined because the time from the date of surgical procedure to the date of radiographic or pathological affirmation of recurrence, loss of life or the final follow-up.
Knowledge assortment
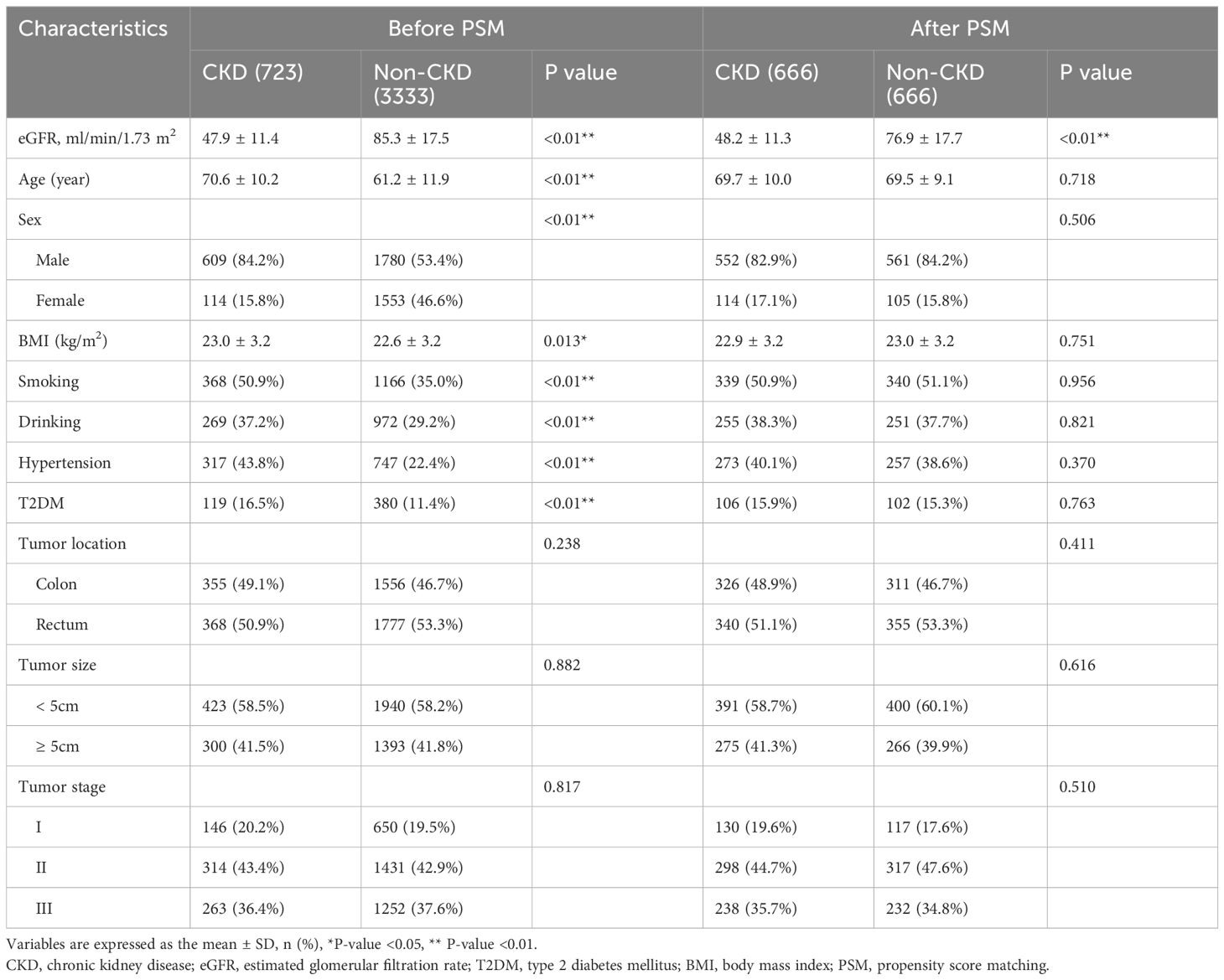
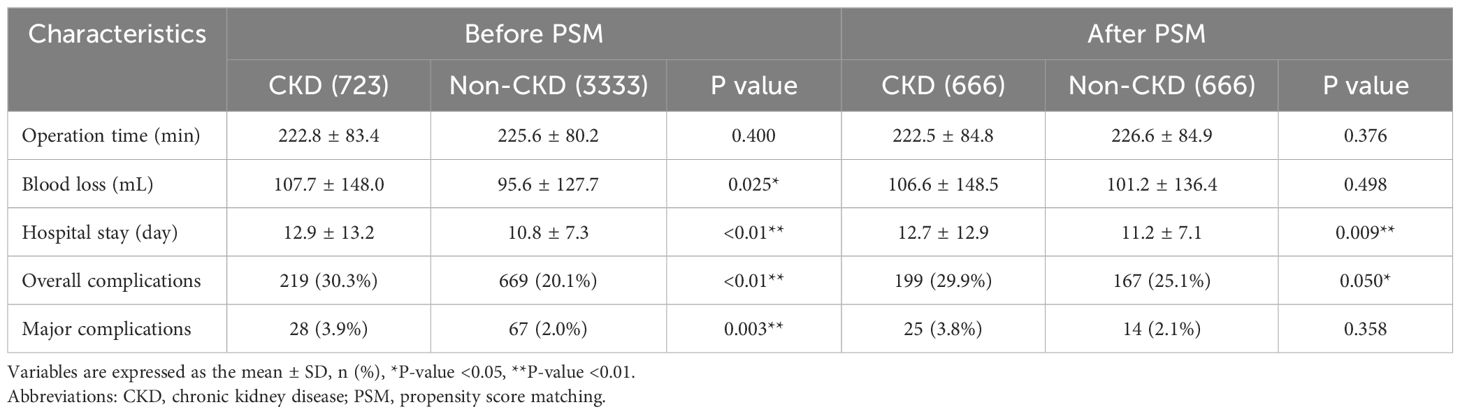
We retrospectively collected baseline info and postoperative short-term outcomes via the inpatient system. Baseline info included age, gender, physique mass index (BMI), smoking and ingesting historical past, hypertension, sort 2 diabetes mellitus (T2DM), tumor location, tumor dimension and tumor stage (Desk 1). Postoperative short-term outcomes included operative time, blood loss, hospital keep, total problems and main problems (Desk 2). Survival knowledge have been primarily obtained via the outpatient follow-up system and phone interviews.
Propensity rating matching (PSM)
Because the grouping of the CKD group and the Non-CKD group was non-random, and variables have been unbalanced. Due to this fact, we used PSM on this examine. Propensity scores are mostly estimated by logistic regression, the place therapy group is taken into account the result and regressed in opposition to noticed baseline traits (21). We initiated a 1:1 (CKD group vs Non-CKD group) matching evaluation by PSM and nearest neighbor matching algorithms and specified a caliper width with 0.01 customary deviation to regulate for variations in baseline traits between the 2 teams. Baseline info for PSM included age, gender, BMI, smoking and ingesting historical past, hypertension, T2DM, tumor location, tumor dimension and tumor stage.
Statistical evaluation
On this article, steady variables have been expressed as imply ± SD, and Frequency variables have been expressed as n (%). We use unbiased samples t-test to investigate variations in eGFR, age, BMI, operation time, blood loss and hospital keep between the CKD group and the Non-CKD group. The chi-square check or Fisher’s actual check was used to investigate variations in intercourse, smoking, ingesting, hypertension, T2DM, tumor location, tumor dimension, tumor stage, total problems and main complication between the CKD group and the Non-CKD group. Moreover, to establish unbiased predictors of OS and DFS, we used the Cox regression evaluation. Firstly, we carried out univariate evaluation for CKD, Intercourse, BMI, T2DM, Tumor web site, Tumor stage, Smokin, Consuming, Hypertension, Tumor dimension, General problems within the two teams, after which multivariate evaluation for elements with P-value <0.05 after univariate evaluation. Knowledge have been analyzed utilizing the SPSS (model 26.0) statistical software program, and a bilateral p-value < 0.05 was thought-about statistically important.
Outcomes
Sufferers
In keeping with the related inclusion and exclusion standards, a complete of 4056 sufferers present process CRC surgical procedure have been lastly included on this evaluation, together with 723 sufferers within the CKD group and 3333 sufferers within the Non-CKD group. After 1:1 PSM, there have been 666 sufferers in every group (Determine 1)
Baseline traits
Earlier than PSM, there have been important variations within the baseline info between the CKD group and the Non-CKD group. The CKD group had older age (P<0.01), the next proportion of male (P<0.01), increased BMI (P=0.013), increased proportions of smoking and ingesting (P<0.01), and extra sufferers with hypertension and T2DM (P<0.01). After 1:1 PSM, there was no important distinction in baseline info between the 2 teams (p>0.05) (Desk 1)
Quick-term outcomes
In contrast the short-term postoperative outcomes between the CKD group and the Non-CKD group, we discovered that the CKD group had extra blood loss (P=0.025), longer postoperative hospital keep (P<0.01), extra total problems (P<0.01) and extra main problems (P=0.003). After PSM, the CKD group nonetheless had an extended postoperative hospital keep (P=0.009) and the next incidence of total problems (p=0.050). CKD won’t have an effect on main problems (P=0.358) (Desk 2).
The incidence of the postoperative problems
This examine counted the postoperative problems with increased morbidity, corresponding to intestinal obstruction, lymphatic fistula, anastomotic fistula, thrombus, postoperative loss of life and pneumonia. Earlier than PSM, the incidence of intestinal obstruction, lymphatic fistula, anastomotic fistula, thrombus, postoperative loss of life and pneumonia within the CKD group was 2.4%, 0.3%, 2.5%, 1.9%, 0.7%, and 6.4%, respectively. The incidence of intestinal obstruction, lymphatic fistula, anastomotic fistula, thrombus, postoperative loss of life and pneumonia within the Non-CKD group was 1.8%, 0.5%, 2.3%, 0.8%, 0.2%, and a couple of.3%, respectively. After PSM, the incidence of intestinal obstruction, lymphatic fistula, anastomotic fistula, thrombus, postoperative loss of life and pneumonia within the CKD group was 2.6%, 0.3%, 2.6%, 2.0%, 0.7%, 5.6%, respectively. The incidence of intestinal obstruction, lymphatic fistula, anastomotic fistula, thrombus, postoperative loss of life and pneumonia within the Non-CKD group was 2.9%, 0.7%, 3.6%, 0.7%, 0.2%, 4.8%, respectively.
Univariate and multivariate evaluation of OS and DFS earlier than and after PSM
The median follow-up time was 33 (1–114) months. Earlier than PSM, by way of OS, age (p<0.01, HR=1.039, 95% CI=1.031–1.048), tumor stage (p<0.01, HR=2.094, 95% CI=1.827–2.401, tumor dimension (p=0.005, HR=1.275, 95% CI=1.075–1.511) and total problems (p<0.01, HR=1.664, 95% CI=1.391–1.990) have been unbiased predictors. Concerning DFS, age (p<0.01, HR=1.028, 95% CI=1.020–1.035), tumor stage (p<0.01, HR=2.022, 95% CI=1.792–2.281), and total problems (p<0.01, HR=1.532, 95% CI=1.300–1.805) have been unbiased predictors. Nevertheless, CKD was not an unbiased predictor of OS or DFS (OS: p=0.440, HR=1.085, 95% CI=0.882–1.335); DFS: p=0.122, HR=1.160, 95% CI=0.961–1.399) (Desk 3).
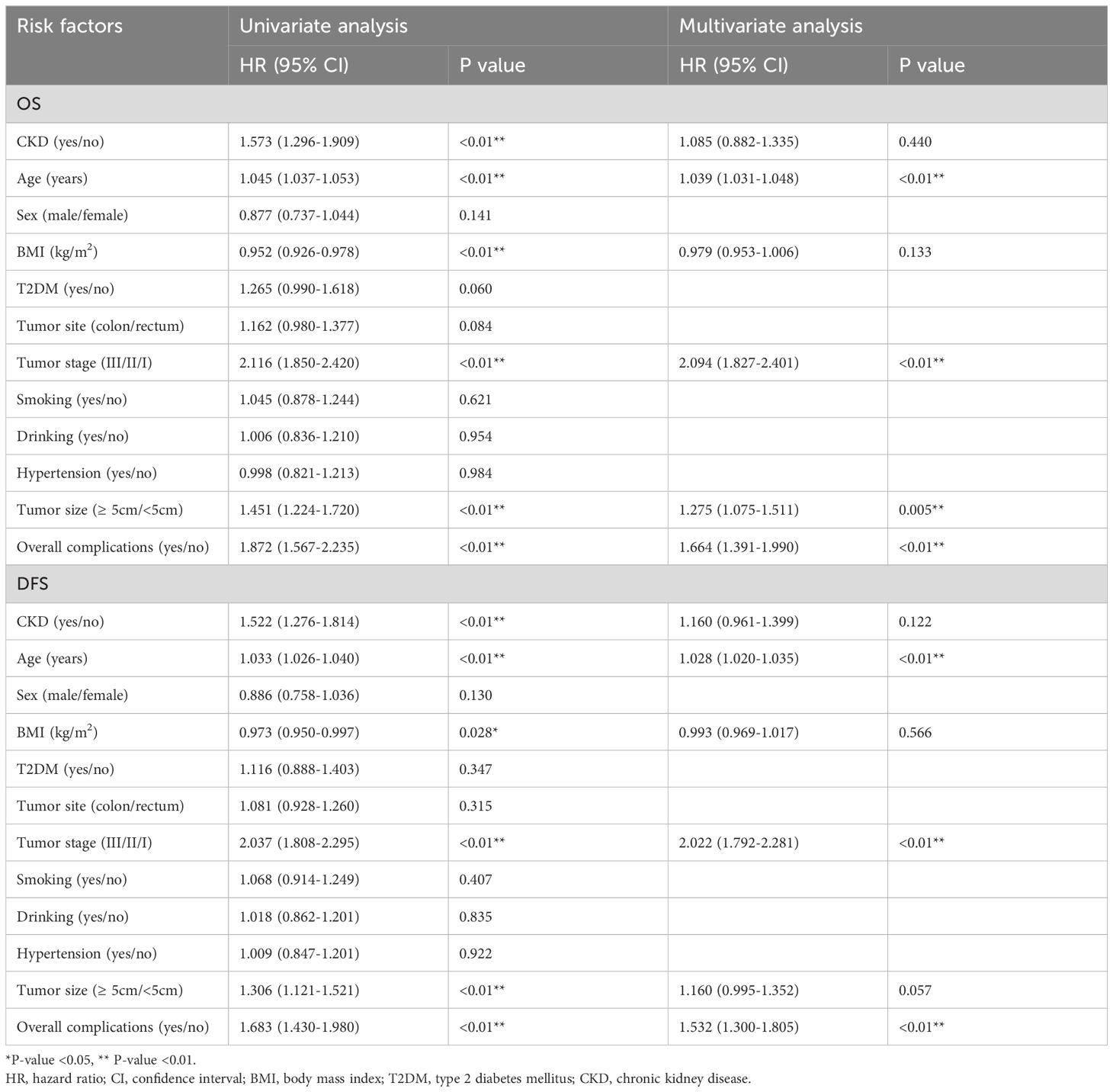
Desk 3 Univariate and multivariate evaluation of total survival of the entire cohort and illness free survival of the entire cohort earlier than PSM.
After PSM, by way of OS, age (p<0.01, HR=1.045, 95% CI=1.028–1.062), tumor stage (p<0.01, HR=1.931, 95% CI=1.564–2.385) and total problems (p<0.01, HR=1.858, 95% CI=1.423–2.425) have been unbiased predictors. Concerning DFS, age (p<0.01, HR=1.034, 95% CI=1.020–1.049), tumor stage (p<0.01, HR=1.852, 95% CI=1.537–2.231), and total problems (p<0.01, HR=1.651, 95% CI=1.295–2.10) have been unbiased predictors. Nevertheless, CKD was not an unbiased predictor of OS or DFS (OS: p=0.619, HR=1.070, 95% CI=0.820–1.396; DFS: p=0.472, HR=1.092, 95% CI=0.859–1.389) (Desk 4).
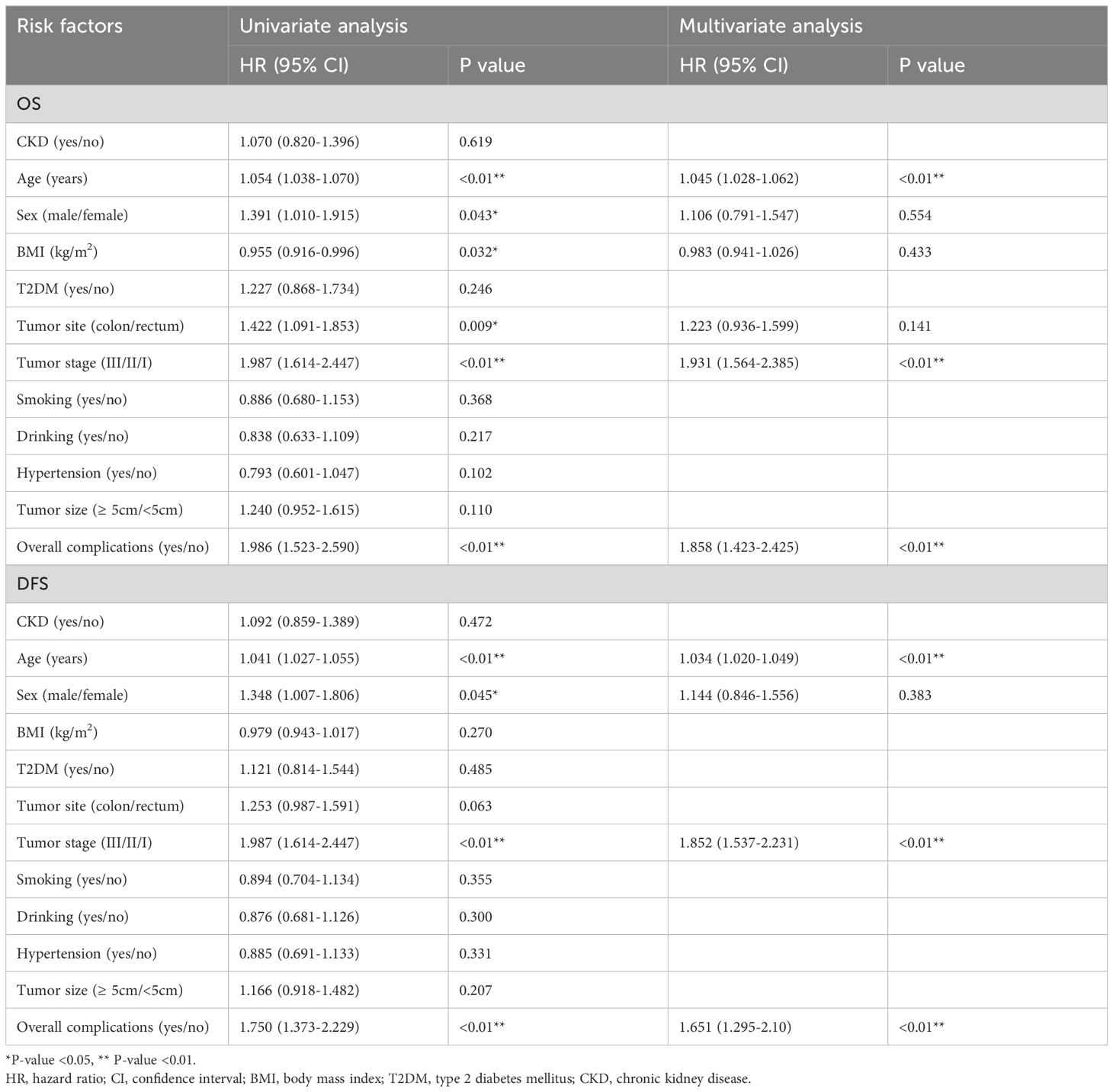
Desk 4 Univariate and multivariate evaluation of total survival of matching cohort and illness free survival of matching cohort after PSM.
Dialogue
A complete of 4056 sufferers with CRC surgical procedure have been included on this evaluation lastly. After PSM, there have been 666 within the CKD group and the Non-CKD group, respectively. After PSM, the CKD group had an extended postoperative hospital keep. Nevertheless, CKD was not an unbiased predictor of OS or DFS.
The impact of CKD on the surgical outcomes has been a sizzling subject. Aune D et al. believed that after cardiac surgical procedure, sufferers with end-stage renal illness had a considerably increased mortality fee than sufferers with regular renal operate (6) Ciriaco P et al. concluded that hemodialysis (HD) sufferers who underwent pneumonectomy had the next incidence of postoperative problems (22); Han IH et al. concluded that sufferers with end-stage renal illness who underwent spinal surgical procedure had increased morbidity and mortality (23). We concluded that CKD was related to an elevated danger of most surgical outcomes, however the impact of CKD on sufferers after CRC surgical procedure was controversial. Some research instructed that CKD elevated postoperative morbidity and mortality in CRC sufferers (12, 13, 24–27). Due to this fact, the aim of this examine was to investigate the impact of CKD on short-term outcomes and prognosis of CRC present process major surgical procedure.
Our examine confirmed that CKD sufferers who underwent CRC surgical procedure had longer hospital stays after harmonizing the variations in baseline knowledge, which was per earlier research (12, 13). Many clinicians believed that the kidneys and the guts have been two organs that interacted with one another (28–31). Research had proven that CKD was related to a considerably elevated danger of myocardial infarction, coronary artery illness, left ventricular hypertrophy and loss of life from cardiac causes (28–32). As well as, CKD led to elevated ranges of inflammatory elements, arterial hypercalcification and endothelial dysfunction (32). All of those mechanisms would possibly contribute to delayed postoperative restoration after surgical procedure, thereby rising the size of hospital keep. Moreover, this endothelial harm might clarify the pro-inflammatory setting in CKD resulting from uremia, malnutrition, quantity overload, or altered calcium and phosphorus metabolism (32). Since inflammatory mediators would possibly result in malignancy via induction of precancerous mutations, adaptive responses, and environmental adjustments (33), this additionally confirmed the affiliation of CKD with the incidence of CRC (7–9).
On this current examine, age, tumor stage, and total problems have been unbiased predictors of OS and DFS, per earlier research (34, 35). Due to this fact, we must always take note of the management of operative problems. Nevertheless, it was value noting that within the PSM evaluation of main postoperative problems, OS and DFS in CRC sufferers, no important distinction was discovered between the CKD group and the Non-CKD group. Regardless that the CKD group confirmed the next total postoperative complication fee earlier than and after PSM, the incidence of main problems was comparable between teams. Regardless of this increased incidence of total problems, the OS and DFS remained comparable between CKD and Non-CKD teams after PSM. Due to this fact, additional analysis is warranted to elucidate the exact impression of CKD on prognosis.
After reviewing the related research, we discovered that though there have been few earlier research on the impact of CKD on CRC surgical procedure, this examine was the primary to make use of PSM to investigate the impression of CKD on the short-term outcomes and prognosis of CRC sufferers. Using PSM drastically diminished variations within the baseline traits and made conclusions extra dependable. And in comparison with typical PSM articles, this examine additionally analyzed pre-matching knowledge, which higher illustrated the impact dimension of potential confounding elements. Nevertheless, this examine additionally had some limitations. First, this was a retrospective single-center examine; second, the follow-up time was comparatively brief; third, this examine solely in contrast the CKD group and the Non-CKD group, and lacked particular staging research of CKD; fourth, our outcomes would possibly nonetheless be biased resulting from choice bias stemming from unbalanced knowledge. Due to this fact, we’re wanting ahead to extra complete multicenter potential randomized managed research to additional verify our findings sooner or later. In future analysis, we additionally wish to use superior methodologies, corresponding to Cox regression with shared frailty, to reinforce the methodological robustness and higher align with the requirements of educational excellence.
In conclusion, CKD extended postoperative hospital keep; nevertheless, CKD won’t have an effect on main postoperative problems, OS or DFS of CRC.
Knowledge availability assertion
The uncooked knowledge supporting the conclusions of this text will likely be made accessible by the authors, with out undue reservation.
Ethics assertion
The research involving people have been permitted by the First Affiliated Hospital of Chongqing Medical College. The research have been carried out in accordance with the native laws and institutional necessities. The contributors offered their written knowledgeable consent to take part on this examine. Written knowledgeable consent was obtained from the person(s) for the publication of any doubtlessly identifiable photographs or knowledge included on this article.
Creator contributions
C-YW: Writing – assessment & modifying. S-PQ: Writing – unique draft. S-QR: Writing – assessment & modifying. Z-XH: Writing – assessment & modifying.
Funding
The creator(s) declare that no monetary assist was acquired for the analysis, authorship, and/or publication of this text.
Acknowledgments
We acknowledge all of the authors whose publications are referred in our article. Particularly, S-QR made an enormous contribution to revise the manuscript. And we thank Xun Lei for the substantial work within the statistical strategies.
Battle of curiosity
The authors declare that the analysis was carried out within the absence of any industrial or monetary relationships that could possibly be construed as a possible battle of curiosity.
The reviewer XZ declared a shared mother or father affiliation with the authors to the dealing with editor on the time of assessment.
Writer’s be aware
All claims expressed on this article are solely these of the authors and don’t essentially symbolize these of their affiliated organizations, or these of the writer, the editors and the reviewers. Any product which may be evaluated on this article, or declare which may be made by its producer, isn’t assured or endorsed by the writer.
References
1. Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, et al. International most cancers statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 nations. CA Most cancers J Clin. (2024) 74:229–63. doi: 10.3322/caac.21834
PubMed Summary | CrossRef Full Textual content | Google Scholar
2. Rawla P, Sunkara T, Barsouk A. Epidemiology of colorectal most cancers: incidence, mortality, survival, and danger elements. Prz Gastroenterol. (2019) 14:89–103. doi: 10.5114/pg.2018.81072
PubMed Summary | CrossRef Full Textual content | Google Scholar
3. Liu XR, Liu F, Li ZW, Liu XY, Zhang W, Peng D. Influence of sort 2 diabetes mellitus on short-term and long-term outcomes of stage iv colorectal most cancers sufferers after major surgical procedure: a propensity rating matching evaluation. Int J Colorectal Dis. (2023) 38:171. doi: 10.1007/s00384-023-04476-9
PubMed Summary | CrossRef Full Textual content | Google Scholar
4. Liu XY, Li ZW, Zhang B, Liu F, Zhang W, Peng D. Results of preoperative bicarbonate and lactate ranges on short-term outcomes and prognosis in aged sufferers with colorectal most cancers. BMC Surg. (2023) 23:127. doi: 10.1186/s12893-023-02039-x
PubMed Summary | CrossRef Full Textual content | Google Scholar
5. Weiner DE, Tighiouart H, Amin MG, Stark PC, MacLeod B, Griffith JL, et al. Continual kidney illness as a danger issue for heart problems and all-cause mortality: a pooled evaluation of community-based research. J Am Soc Nephrol. (2004) 15:1307–15. doi: 10.1097/01.ASN.0000123691.46138.E2
PubMed Summary | CrossRef Full Textual content | Google Scholar
6. Aune D, Solar X, Nie J, Huang W, Liao B, Wang Y. Self-reported power kidney illness and the danger of all-cause and cause-specific mortality: outcome-wide affiliation examine of 54 causes of loss of life within the Nationwide Well being Interview Survey. BMC Nephrol. (2022) 23:165. doi: 10.1186/s12882-022-02771-1
PubMed Summary | CrossRef Full Textual content | Google Scholar
7. Zhang B, Liu XR, Liu XY, Kang B, Yuan C, Liu F, et al. The impression of serum parameters related to kidney operate on the short-term outcomes and prognosis of colorectal most cancers sufferers present process radical surgical procedure. Can J Gastroenterol Hepatol. (2023) 2023:2017171. doi: 10.1155/2023/2017171
PubMed Summary | CrossRef Full Textual content | Google Scholar
8. Aashima Nanda M, Sharma R, Jani C. The burden of power kidney illness in asia, 1990-2019: examination of estimates from international burden of illness 2019 examine. Nephrol (Carlton). (2022) 27:610–20. doi: 10.1111/nep.14051
9. Li ZW, Zhang B, Liu XY, Kang B, Liu XR, Yuan C, et al. The impact of bilirubin on scientific outcomes of sufferers with colorectal most cancers surgical procedure: A ten-year quantity single-center retrospective examine. Nutr Most cancers. (2023) 75:1315–22. doi: 10.1080/01635581.2023.2170430
PubMed Summary | CrossRef Full Textual content | Google Scholar
10. Wu MY, Chang TC, Chao TY, Huang MT, Lin HW. Threat of colorectal most cancers in power kidney illness: a matched cohort examine primarily based on administrative knowledge. Ann Surg Oncol. (2013) 20:3885–91. doi: 10.1245/s10434-013-3065-8
PubMed Summary | CrossRef Full Textual content | Google Scholar
12. Komaki Y, Komaki F, Micic D, Ido A, Sakuraba A. Threat of colorectal most cancers in power kidney illness: A scientific assessment and meta-analysis. J Clin Gastroenterol. (2018) 52:796–804. doi: 10.1097/MCG.0000000000000880
PubMed Summary | CrossRef Full Textual content | Google Scholar
13. Currie A, Malietzis G, Askari A, Nachiappan S, Swift P, Jenkins JT, et al. Influence of power kidney illness on postoperative consequence following colorectal most cancers surgical procedure. Colorectal Dis. (2014) 16:879–85. doi: 10.1111/codi.12665
PubMed Summary | CrossRef Full Textual content | Google Scholar
14. Huang CS, Huang LK, Chen CY, Wang WS, Yang SH. Prognostic worth of postoperative serum carcinoembryonic antigen ranges in colorectal most cancers sufferers with power kidney illness. Am J Surg. (2021) 221:162–7. doi: 10.1016/j.amjsurg.2020.07.015
PubMed Summary | CrossRef Full Textual content | Google Scholar
15. Nozawa H, Kitayama J, Sunami E, Watanabe T. Influence of power kidney illness on outcomes of surgical resection for major colorectal most cancers: a retrospective cohort assessment. Dis Colon Rectum. (2012) 55:948–56. doi: 10.1097/DCR.0b013e3182600db7
PubMed Summary | CrossRef Full Textual content | Google Scholar
17. Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF third, Feldman HI, et al. A brand new equation to estimate glomerular filtration fee. Ann Intern Med. (2009) 150:604–12. doi: 10.7326/0003-4819-150-9-200905050-00006
PubMed Summary | CrossRef Full Textual content | Google Scholar
18. Nationwide Kidney Basis. Ok/DOQI scientific follow tips for power kidney illness: analysis, classification, and stratification. Am J Kidney Dis. (2002) 39:S1–266.
20. Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien-Dindo classification of surgical problems: five-year expertise. Ann Surg. (2009) 250:187–96. doi: 10.1097/SLA.0b013e3181b13ca2
PubMed Summary | CrossRef Full Textual content | Google Scholar
21. Austin PC. An introduction to propensity rating strategies for decreasing the results of confounding in observational research. Multivariate Behav Res. (2011) 46:399–424. doi: 10.1080/00273171.2011.568786
PubMed Summary | CrossRef Full Textual content | Google Scholar
22. Ciriaco P, Casiraghi M, Melloni G, Carretta A, Libretti L, Augello G, et al. Pulmonary resection for non-small-cell lung most cancers in sufferers on hemodialysis: scientific consequence and long-term outcomes. World J Surg. (2005) 29:1516–9. doi: 10.1007/s00268-005-0047-4
PubMed Summary | CrossRef Full Textual content | Google Scholar
23. Han IH, Kim KS, Park HC, Chin DK, Jin BH, Yoon YS, et al. Spinal surgical procedure in sufferers with end-stage renal illness present process hemodialysis remedy. Backbone (Phila Pa 1976). (2009) 34:1990–4. doi: 10.1097/BRS.0b013e3181abbdff
PubMed Summary | CrossRef Full Textual content | Google Scholar
25. Chiang SF, Chen JS, Tang R, Yeh CY, Hsieh PS, Tsai WS, et al. The impression of kidney operate on colorectal most cancers sufferers with localized and regional ailments: An observational examine from Taiwan. Indian J Most cancers. (2019) 56:241–7. doi: 10.4103/ijc.IJC_294_18
PubMed Summary | CrossRef Full Textual content | Google Scholar
26. Mirnezami A, Mirnezami R, Chandrakumaran Ok, Sasapu Ok, Sagar P, Finan P. Elevated native recurrence and diminished survival from colorectal most cancers following anastomotic leak: systematic assessment and meta-analysis. Ann Surg. (2011) 253:890–9. doi: 10.1097/SLA.0b013e3182128929
PubMed Summary | CrossRef Full Textual content | Google Scholar
27. Dudani S, Marginean H, Gotfrit J, Tang PA, Monzon JG, Dennis Ok, et al. The impression of power kidney illness in regionally superior rectal most cancers sufferers handled with neoadjuvant chemoradiation. J Clin Oncol. (2018) 36:794–4. doi: 10.1200/JCO.2018.36.4_suppl.794
30. Tonelli M, Wiebe N, Culleton B, Home A, Rabbat C, Fok M, et al. Continual kidney illness and mortality danger: a scientific assessment. J Am Soc Nephrol. (2006) 17:2034–47. doi: 10.1681/ASN.2005101085
PubMed Summary | CrossRef Full Textual content | Google Scholar
31. Wali RK, Wang GS, Gottlieb SS, Bellumkonda L, Hansalia R, Ramos E, et al. Impact of kidney transplantation on left ventricular systolic dysfunction and congestive coronary heart failure in sufferers with end-stage renal illness. J Am Coll Cardiol. (2005) 45:1051–60. doi: 10.1016/j.jacc.2004.11.061
PubMed Summary | CrossRef Full Textual content | Google Scholar
32. Gansevoort RT, Correa-Rotter R, Hemmelgarn BR, Jafar TH, Heerspink HJ, Mann JF, et al. Continual kidney illness and cardiovascular danger: epidemiology, mechanisms, and prevention. Lancet. (2013) 382:339–52. doi: 10.1016/S0140-6736(13)60595-4
PubMed Summary | CrossRef Full Textual content | Google Scholar
33. Shacter E, Weitzman SA. Continual irritation and most cancers. Oncol (Williston Park). (2002) 16:217–26.
34. Liu XY, Kang B, Cheng YX, Yuan C, Tao W, Zhang B, et al. The short-term and oncologic outcomes of youthful VS older colorectal most cancers sufferers present process major surgical procedure: a propensity rating matching evaluation. BMC Most cancers. (2022) 22:153. doi: 10.1186/s12885-022-09246-4
PubMed Summary | CrossRef Full Textual content | Google Scholar
35. Huh JW, Lee WY, Park YA, Cho YB, Kim HC, Yun SH, et al. Oncological consequence of surgical web site an infection after colorectal most cancers surgical procedure. Int J Colorectal Dis. (2019) 34:277–83. doi: 10.1007/s00384-018-3194-4
PubMed Summary | CrossRef Full Textual content | Google Scholar